Basal Cell Carcinoma
BCC can appear on the skin in various ways, including red patches, pink growths, open sores, and shiny bumps. Overexposure to ultraviolet (UV) rays is the most common cause. With proper treatment, BCC is rarely life-threatening.
Approximately three million people are diagnosed with BCC each year. The condition is most common among individuals exposed to high levels of UV rays. Although the average age of BCC patients is decreasing, it remains most prevalent in people over the age of 40.
Examples of Basal Cell Carcinoma
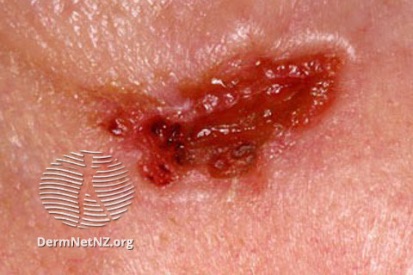
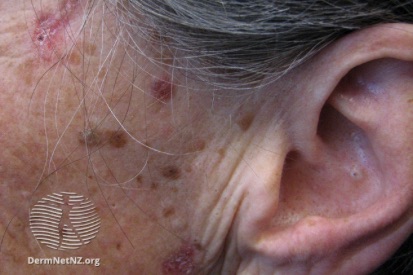
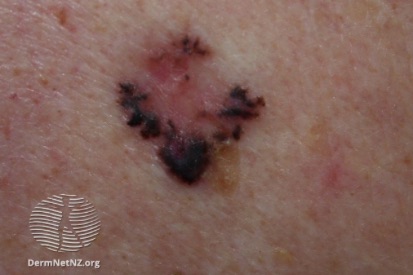
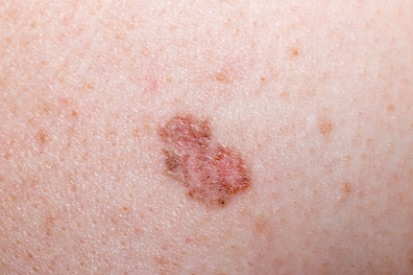
Symptoms of Basal Cell Carcinoma
Basal cell carcinoma (BCC) is the most common form of skin cancer and often develops in areas of the body that are frequently exposed to the sun. Basal cell carcinoma on the face is particularly common. Other frequent sites include the neck, scalp, and arms. Early-stage basal cell carcinoma can be subtle and may resemble non-threatening skin conditions.
BCC typically presents as slow-growing lesions that rarely cause pain but may become problematic over time if untreated. These lesions may look like shiny, pearly bumps, open sores that don’t heal, or flat, scar-like areas. It's essential to consult a dermatologist if you notice any persistent or changing spots on your skin.
Common signs and symptoms of BCC include:
- A pearly or waxy bump, often with visible blood vessels
- A flat, flesh-colored, or brown scar-like lesion
- An open sore that bleeds, oozes, or crusts and remains open for weeks
- A pink growth with a slightly raised, rolled border and a crusted indentation in the center
- A red patch that may itch or hurt
- Lesions developing on sun-exposed areas like the face, ears, neck, scalp, shoulders, and back
Causes of Basal Cell Carcinoma
The primary cause of BCC is prolonged exposure to ultraviolet (UV) radiation from the sun or tanning beds. Those over the age of 40 are also more susceptible to BCC. While anyone can develop it, certain risk factors increase the likelihood, including genetics and skin type.
Common causes of BCC include:
- Chronic sun exposure, especially as a child, without protection
- Use of tanning beds
- Fair skin, light eyes, and blond or red hair
- A history of severe sunburns, especially in childhood
- A family history of skin cancer
- Genetic conditions, such as basal cell nevus syndrome
- A weakened immune system due to illness or medication
Preventing Basal Cell Carcinoma
While basal cell cancer is most often caused by cumulative sun exposure, many cases can be prevented or caught early with the right habits. Practicing sun protection year-round and regular skin checks can help reduce risk. Understanding what BCC looks like, especially in the early stages, is critical for catching it before it becomes severe.
Common preventative measures include:
- Using a broad-spectrum sunscreen with SPF 30 or higher daily, even on cloudy days
- Avoiding sun exposure during peak hours (10 AM – 4 PM)
- Wearing protective clothing, wide-brimmed hats, and UV-blocking sunglasses when outdoors
- Staying in the shade whenever possible, especially during midday
- Avoiding tanning beds, which significantly increase skin cancer risk
- Performing regular self-skin checks and being aware of BCC symptoms, such as shiny bumps, open sores, or scar-like patches
- Learning to recognize what basal cell carcinoma looks like using credible resources and basal cell carcinoma pictures of the early stages
- Scheduling annual total body skin examinations with a dermatologist for professional screening
Basal Cell Carcinoma FAQs
Preventing BCC involves protecting your skin from UV radiation by using sunscreen, wearing protective clothing, seeking shade, and avoiding tanning beds. Regular skin checks and self-examinations are also important.
Yes, BCC can recur, especially if not completely removed. Regular follow-up appointments with a dermatologist are essential to monitor for any new or returning lesions.
BCC can appear as a shiny bump, a red patch, a pink growth, an open sore, or a scar-like area on the skin. These lesions may bleed, ooze, or crust and do not heal over time.
The primary cause of BCC is long-term exposure to ultraviolet (UV) radiation from the sun or tanning beds. Other risk factors include fair skin, a history of sunburns, and a family history of skin cancer.
Anyone can develop BCC, but those at higher risk include individuals with fair skin, light hair, and light eyes, those with a history of sunburns or excessive sun exposure, and those with a personal or family history of skin cancer.
If you notice any unusual or persistent changes in your skin, schedule an appointment with a dermatologist for an evaluation. Early detection and treatment are key to managing BCC effectively.
From Our QualDerm Family of Brands: Non-Melanoma Skin Cancers
How to Treat Basal Cell Carcinoma
Treatment for BCC depends on several factors, including the size, depth, and location of the lesion, as well as the patient’s overall health. With various effective approaches available, from surgical options to newer non-invasive therapies, it’s crucial to tailor the treatment to each case. Early intervention can improve outcomes and minimize scarring. Whether the goal is basal skin carcinoma removal or long-term management, knowing the range of available treatments is essential.
Non-Surgical Treatments
There are several non-surgical treatment options for patients who are not candidates for surgery or prefer less invasive approaches. These include topical medications such as imiquimod or 5-fluorouracil, which can be effective for superficial BCCs.
Basal cell carcinoma radiation treatment may be recommended for older adults or those with tumors in difficult-to-operate locations. Electrodesiccation and curettage involve numbing the area, scraping off the lesion, and cauterizing it to destroy remaining tumor cells and control bleeding. Cryotherapy is another option, which freezes the lesion with liquid nitrogen. Additionally, superficial radiation therapy (SRT) treatment for skin cancer is emerging as a non-invasive alternative for certain patients, particularly for low-risk lesions.
Surgical Procedures
Surgery remains the most common and effective option for basal cell carcinoma treatment. Excisional surgery involves cutting out the cancerous lesion along with a small margin of healthy tissue to ensure complete removal. Another highly effective technique is Mohs surgery for basal cell carcinoma, especially used for facial areas or lesions with a high risk of recurrence.
This precise method involves removing the cancer layer by layer while examining each layer under a microscope, ensuring minimal damage to surrounding healthy skin. Mohs surgery offers the highest cure rates, around 98% for primary, non-recurrent BCC, while preserving healthy tissue and delivering excellent cosmetic outcomes.
New and Emerging Treatments
Advancements in skin cancer treatment have led to promising new therapies for basal cell carcinoma. Targeted drugs such as hedgehog pathway inhibitors are used for advanced or recurrent cases that don’t respond well to conventional treatment. Immunotherapy and photodynamic therapy are also being explored in clinical settings for patients who need alternatives to traditional basal cell carcinoma surgery.
Topical therapeutic options, including certain creams or ointments, may also be considered for specific lesions. Your dermatologist will discuss these based on the characteristics of your basal cell carcinoma.
Featured Products for Sun Protection
Check your local office for current stock!
Check your local office for current stock!
